A Scientific Inquiry into Heart Rhythms, Sleep, and Stress Biomarkers
What if heartbeat could reveal your resilience to stress?
Could the structure of sleep predict vulnerability to depression?
And can the skin signal distress before someone even feel it?
These aren’t speculative questions. They reflect recent growing evidence that physiological signals can serve as early indicators of emotional health. From heart rate variability (HRV) to biochemical markers like electrodermal activity (EDA), our internal systems hold data about how well we regulate, recover, and respond emotionally.
This article explores the mechanisms, biological bases, and research findings connecting physiology and emotion, with a focus on HRV, sleep architecture, and stress biomarkers.
1. Heart Rate Variability (HRV) and Emotion Regulation
What is HRV?
Heart Rate Variability (HRV) refers to the variation in time intervals between successive heartbeats. Unlike heart rate (beats per minute), HRV captures the dynamic balance between sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) systems of the autonomic nervous system (ANS).
- High HRV: Reflects a flexible and responsive autonomic system
- Low HRV: Indicates rigidity, chronic stress, or poor emotional regulation

Source: Team, L. (2022, February 2). Why HRV be The Important Mental Health Indicator – Lief Blog. Lief Blog. https://blog.getlief.com/why-hrv-be-the-most-important-mental-health-indicator/
HRV represents the temporal variation between successive heartbeats and reflects the balance of sympathetic and parasympathetic activity within the autonomic nervous system (ANS). High resting-state HRV is associated with greater emotional regulation capacity, cognitive flexibility, and lower psychiatric symptomatology.
Theoretical Framework
Thayer et al. (2009) introduced the Neurovisceral Integration Model, linking HRV to central autonomic network activity, particularly the prefrontal cortex, anterior cingulate, and amygdala. These areas modulate emotional responses, and their regulatory efficiency correlates with HRV amplitude.
The Neurovisceral Integration Model (Thayer et al.) connects HRV to higher-order brain structures, specifically the prefrontal cortex, which modulates emotional responses via inhibitory projections to the amygdala and brainstem. HRV, therefore, reflects top-down regulation of emotion.
Functional MRI studies confirm that individuals with higher resting HRV show:
- Greater prefrontal activity during emotional tasks
- Better amygdala inhibition under stress
Enhanced executive function and emotional flexibility
Research Highlights
A meta-analysis of HRV biofeedback studies (HeartMath Institute, 2022) involving over one million data points shows that resonant frequency breathing improves HRV coherence and correlates with reductions in anxiety, depressive symptoms, and perceived stress.
- HRV biofeedback interventions improved HRV coherence and reduced anxiety and depressive symptoms (HeartMath Institute, 2022)
- Low HRV predicts poorer outcomes in emotion-focused therapy, even after controlling for baseline psychological symptoms
Possible Clinical implication:
HRV should be incorporated into routine psychological assessments to quantify autonomic flexibility and emotional regulation capacity. Biofeedback interventions targeting HRV coherence are evidence-supported adjuncts to psychotherapy.
HRV Biofeedback: Training Automatic Flexibility
While HRV is a passive measure of autonomic regulation, it can also be an active target for intervention. A growing body of research supports HRV biofeedback (HRVB) as an effective method to enhance vagal tone and improve emotional outcomes.
What is HRV Biofeedback?
HRVB involves paced breathing, real-time feedback, and resonant frequency training to promote parasympathetic engagement. Typically, individuals are trained to breathe at a frequency (~6 breaths/min) that maximizes HRV amplitude.
Evidence for Effectiveness
A meta-analysis of 24 randomized controlled trials showed that HRVB significantly reduces symptoms of stress and anxiety, with a mean effect size (Cohen’s d) > 0.80, which is notably higher than traditional CBT (~0.70) or first-line anxiolytic pharmacotherapy (~0.60).
Other applications include:
- Major depressive disorder: HRVB increases prefrontal regulatory activity and reduces affective lability
- Substance use disorders: Improved interoceptive awareness and impulse regulation
- PTSD: Modulation of hyperarousal symptoms and improved sleep quality
These findings suggest HRVB is not only effective, but also non-invasive, cost-efficient, and easily scalable with digital technologies.
Broader Implications
Given the projected global burden of mental illness, which by some estimates will surpass all physical diseases in disability-adjusted life years (DALYs) by 2030, there is increasing urgency to explore scalable, physiological interventions.
As HRVB protocols continue to evolve, especially through mobile platforms and wearables, they offer a promising pathway for population-level emotional resilience training.
2. Sleep Architecture as an Emotional Predictor
Sleep is structured into non-REM (NREM) and REM (Rapid Eye Movement) phases. NREM includes deep slow-wave sleep (SWS), while REM sleep is marked by vivid dreams and high brain activity.
Each stage plays distinct roles:
- REM sleep: Emotional memory integration; increased limbic activity
- SWS: Synaptic downscaling and emotional reset; promotes PFC-limbic regulation
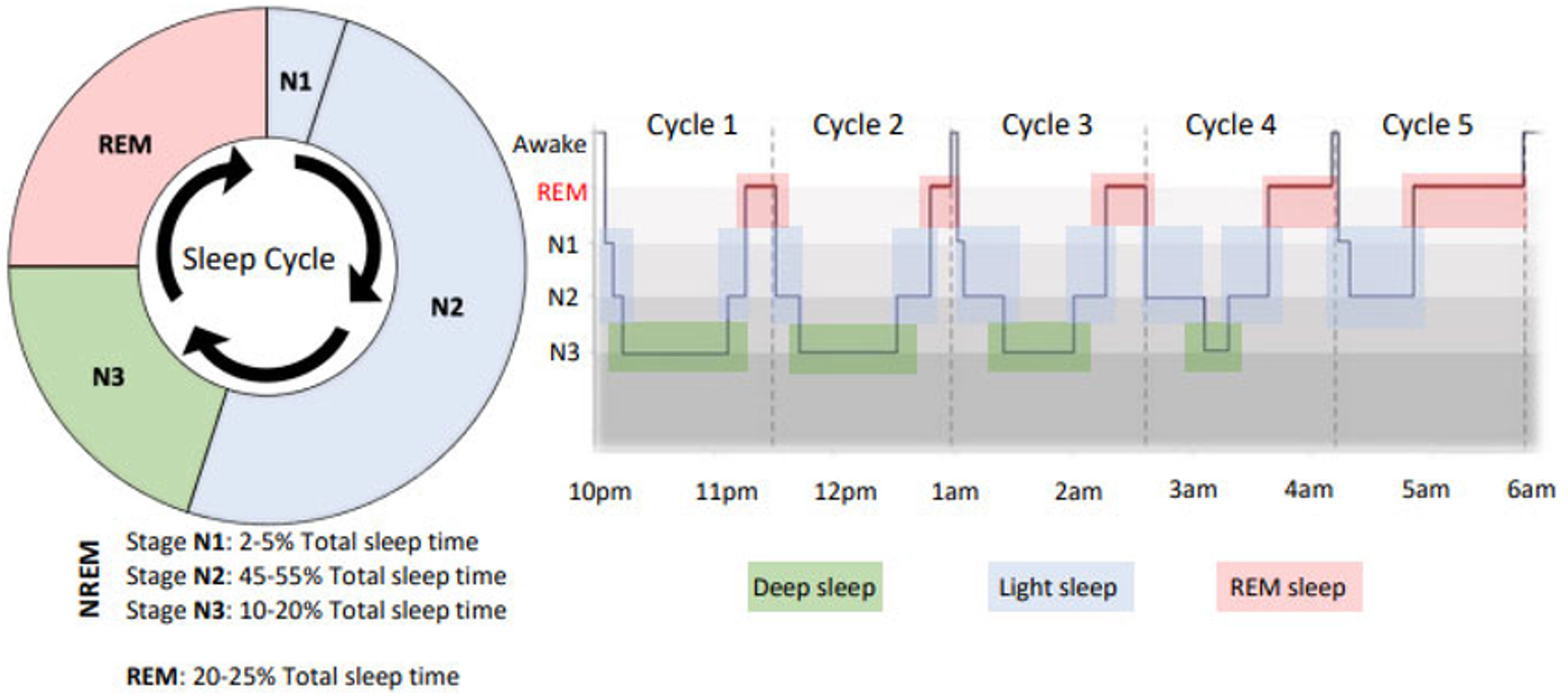
Source: Sleep “architecture”, which shows the typical percentage of time spent.
How Sleep Refelcts Emotional Vulnerability
Disruptions in this structure often precede or accompany emotional disorders:
- Increased REM density and shortened REM latency are predictors of depression and are associated with increased vulnerability to mood disorders.
- Reduced SWS impairs emotional reactivity control and increases anxiety sensitivity
These changes are not just correlational. Experimental REM deprivation heightens amygdala reactivity by up to 60%, particularly in response to negative stimuli (APA, 2023).
Neurobiological Insights
REM sleep supports the reconsolidation of affective memories, whereas SWS is crucial for neural recovery and emotional homeostasis. Dysregulation in either stage alters activity in the ventromedial prefrontal cortex, amygdala, and default mode network, regions implicated in depression and anxiety (Palmer & Alfano, 2023).
Research Highlights
- Shortened REM latency and increased REM density predict major depressive episodes (Palmer & Alfano, 2023).
- A 2023 APA review shows that 24–48 hours of sleep deprivation results in heightened amygdala activation, blunted prefrontal inhibition, and increased affective lability.
- Longitudinal sleep EEG studies show altered REM patterns precede first depressive episodes
- REM-dominant sleep during emotional processing impairs extinction learning, a mechanism critical in PTSD and anxiety
Possible Clinical implication:
Sleep metrics (via PSG or actigraphy) should be monitored in patients presenting with affective instability. Sleep-focused interventions may offer both preventive and corrective emotional stabilization.
3. Electrodermal Activity: Real-Time Emotional Feedback
EDA measures sweat-induced conductance changes via eccrine gland activation under sympathetic control. Its non-invasive nature and millisecond precision make it a valuable tool in detecting emotional arousal and anticipatory anxiety.
- Phasic changes (Skin Conductance Response): Triggered by stimuli
- Tonic levels (Skin Conductance Level): Baseline emotional arousal
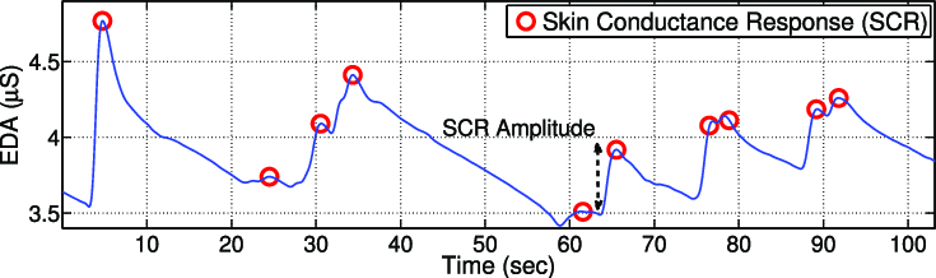
Source: Example of an electrodermal activity (EDA) signal of skin conductance.
Research Highlights:
- In a machine learning–augmented study, Gonçalves et al. (2018) showed that EDA signal fusion with EEG and facial EMG enabled over 85% accuracy in emotion classification tasks.
- EDA-based models achieve >85% accuracy in emotion recognition, especially in stress-detection applications.
Possible Clinical implication:
EDA should be considered for integration into multi-modal emotional state monitoring systems, especially in high-risk or treatment-resistant populations.
4. Clinical Integration: Toward a Multimodal Assessment Model
Incorporating HRV, sleep metrics, and biochemical markers into routine clinical practice provides a data-driven framework for early detection and precision treatment planning. Emerging clinical platforms are beginning to leverage wearable sensors, AI-driven analytics, and real-time biofeedback to support this shift.
Cutting-Edge Directions
- Longitudinal tracking of HRV and sleep alongside mood diaries
- Machine learning models integrating EDA, facial affect, and speech prosody
- Biofeedback devices combining HRV and galvanic skin response for home-based intervention
References
- Thayer, J. F., et al. (2009). Heart rate variability and self-regulation: Ann Behav Med, 37(2), 141–153.
- HeartMath Institute. (2022). HRV Coherence and Emotional States.
- Palmer, C. A., & Alfano, C. A. (2023). Sleep, 46(7), zsad068.
- American Psychological Association. (2023). Impact of Sleep Loss on Emotion.
- Frontiers in Behavioral Neuroscience. (2022). Cortisol and Emotional Distress.
- Gonçalves, J., et al. (2018). Deep Multimodal Emotion Recognition. IEEE Transactions on Affective Computing.

